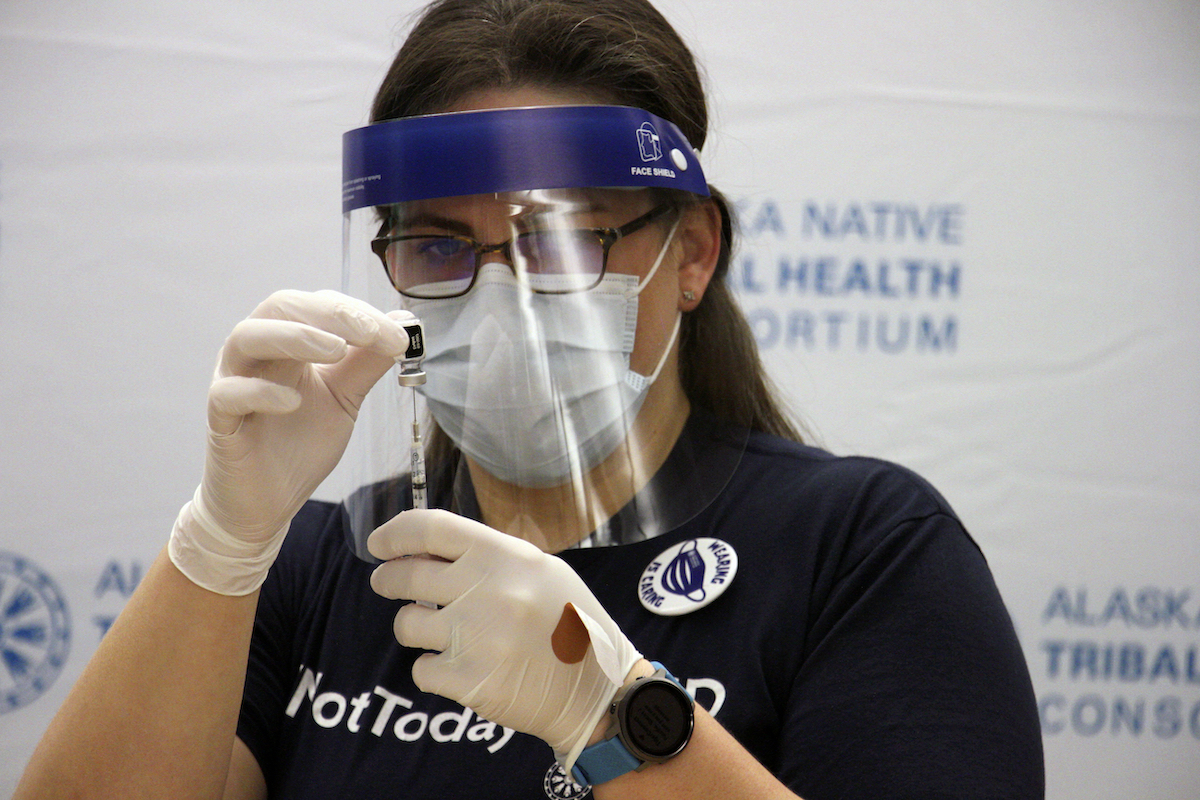
Native Americans and Alaskan Natives are dying at almost twice the rate of white Americans, according to detailed analysis by APM Research Lab—an independent research and data assessment organization.
According to APM’s recently published study, one in every 475 Native Americans has died from COVID since the start of the pandemic, compared with one in every 825 white Americans and one in every 645 Black Americans, nationwide.
The true death toll may be significantly higher as multiple states and cities provide patchy or no data on Native Americans deaths to COVID-19. Of those that do, communities in Mississippi, New Mexico, Arizona, Montana, Wyoming and the Dakotas have been the hardest hit.
The findings are part of the Lab’s Color of Coronavirus project which indicates clearly that Native American communities have had demonstrably higher rates of infection and mortality since the pandemic began. According to the report, Native Americans have suffered 211 deaths per 100,000 people, compared with 121 white Americans per 100,000.
The Pacific Northwest has not been immune to this disproportionate rate, according to Victoria Warren-Mears—the Director of the Northwest Tribal Epidemiology Center at the Northwest Portland Area Indian Health Board (NPAIHB).
The NPAIHB is a tribal organization founded in 1972 by the tribes of Idaho, Oregon and Washington State for health advocacy.
When asked about Oregon’s COVID-19 response for the Indigenous peoples residing in the state, and elsewhere in the Pacific Northwest, Dr. Warren-Mears said, “The nine tribes of Oregon and the urban program are actively collaborating with the state of Oregon on topics around COVID-19. This includes information around testing and vaccine distribution.”
The data available in state tracking systems for Oregon is among the nation’s best, largely due to the Race, Ethnicity, Language and Disability (REAL-D) requirements to report race, ethnicity, language and disability status with testing and vaccination.
According to the Oregon State government’s official website, in 2020, Oregon legislature passed a law requiring health care providers to “collect REALD information at health care visits related to COVID-19, and [to] share this information with the Oregon Health Authority (OHA).”
“In Oregon, less than 18% of that type of data is missing, which is less missing data than many other states,” Warren-Mears said. “I think primary concerns are continued vaccine distribution in an environment where there simply are not enough vaccines available to meet all of the demand for vaccines in the state. This is a national supply issue, and as additional vaccines are approved for emergency use, this lack of supply should resolve.”
Assurances aside, vaccines are still difficult to come by for Native communities and people of color in Oregon—and across the country—according to APM Research Lab’s analysis.
When asked about why COVID-19 has affected Native American populations disproportionately, Warren-Mears spoke to accessibility. “The health care availability to tribes and urban Indians has been underfunded since its inception,” she said. “This has led to long term inequities in health.”
The Centers for Disease Control and Prevention (CDC) has an index that describes those at most risk called the Social Vulnerability Index (SVI). Looking at this, the most vulnerable areas often correspond to tribal and urban areas with high concentrations of Native American and Alaska Native peoples. These social determinants of health are some of the root causes of increased illness and death.
According to the federal Indian Health Service (IHS) department, “American Indians and Alaska Natives continue to die at higher rates than other Americans in many categories, including chronic liver disease and cirrhosis, diabetes mellitus, unintentional injuries, assault/homicide, intentional self-harm/suicide and chronic lower respiratory diseases.”
The national figures show that, even though more infectious variants have yet to take hold in the United States, the situation has already had a devastating toll on Native communities, and may get worse.
“A primary issue that still persists is the loss of revenue for clinics when they switched to providing more emergent care, testing for COVID-19, caring for patients and now vaccination,” Warren-Mears said. “There is a shortage in many tribes of an adequate number of health care providers to provide pandemic services and provide the routine health care programs that are so essential. It is unclear how the inadequate staffing and funding will impact the future.”
“Overall, the tribes and urban programs in Oregon have done an outstanding job of responding to the pandemic. I have no doubt that they will continue to do so. Primarily, we need to get vaccines into as many arms as possible right now and try to stay ahead of the viral mutations,” Warren-Mears concluded.
Last month was the deadliest so far in the U.S., with 958 total recorded Native deaths—a 35% increase since December. For white Americans, deaths rose by 10% over the same period.
A recent Lancet study indicates that under the Trump administration’s response to COVID-19, nearly 40% of deaths could have been avoided, due to policy mistakes and the like.